Accelerate Provider Enrollment for a Faster Path to Revenue
Stop losing months of revenue to enrollment delays. Track payer status in real-time and position your organization for delegated credentialing to cut wait times by 90%.


How We Help You Manage the Complexities of Provider Enrollment
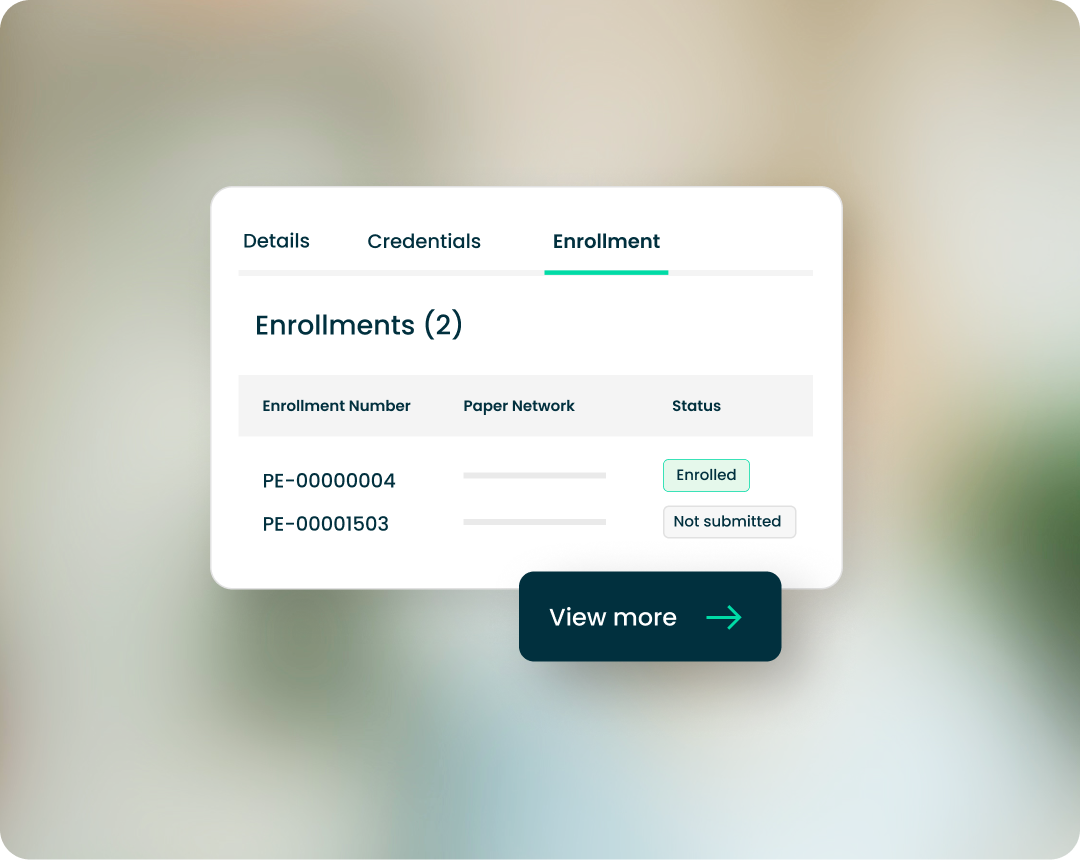
Consolidated Reporting
Bring enrollment management into the same place you do credentialing—eliminating redundancies and increasing process visibility.

Database Hierarchy
Show you all enrollments associated with a provider, providers associated with payer groups, and more.

Key Dates Tracking and Task Management
Keep track of important dates such as submitted, effective, and revalidation, while automating task creation for reminders and follow ups.

Greater Insights with Dashboard Views
View enrollments at a glance with pre-built dashboards for insight into enrollment statuses, and communications.
Generate Enrollment Rosters in Minutes, Not Days
Stop wasting hours manually formatting spreadsheets for every payer. Verifiable simplifies the process by automating roster generation, ensuring your delegated partners receive accurate, compliant data instantly.
Configurable Roster
Templates
Drag and drop data fields to create reusable templates that match the unique formatting requirements of each health plan. Build it once, and generate compliant files forever.
One-Click Report
Generation
Accelerate your submissions by instantly downloading roster reports via CSV. Eliminate manual copy-pasting errors that lead to enrollment kickbacks and delays.
Active Enrollment
Tracking
Organize enrollment data by health plan and track effective dates to maintain accurate visibility into your active rosters. Filter by status to see exactly who is enrolled and who is pending.
Streamlined
Updates
Easily include summarized changes (adds, terms, and updates) in your reports to ensure payers process your network changes quickly and accurately.
Connect Enrollment to Your Revenue Cycle
Feeding provider data directly into Salesforce or into your system of choice using Verifiable’s APIs means enrollment data isn't siloed.
Unified Data
Enrollment status updates instantly on the Provider Record, visible to contracting, billing, and provider relations teams.
Prevent Denials
Ensure billing teams only submit claims for providers who are fully "Par" (Participating) and effective, reducing backend denials.

.svg)

